The Link Between Diabetes and Peripheral Artery Disease (PAD): What You Need to Know
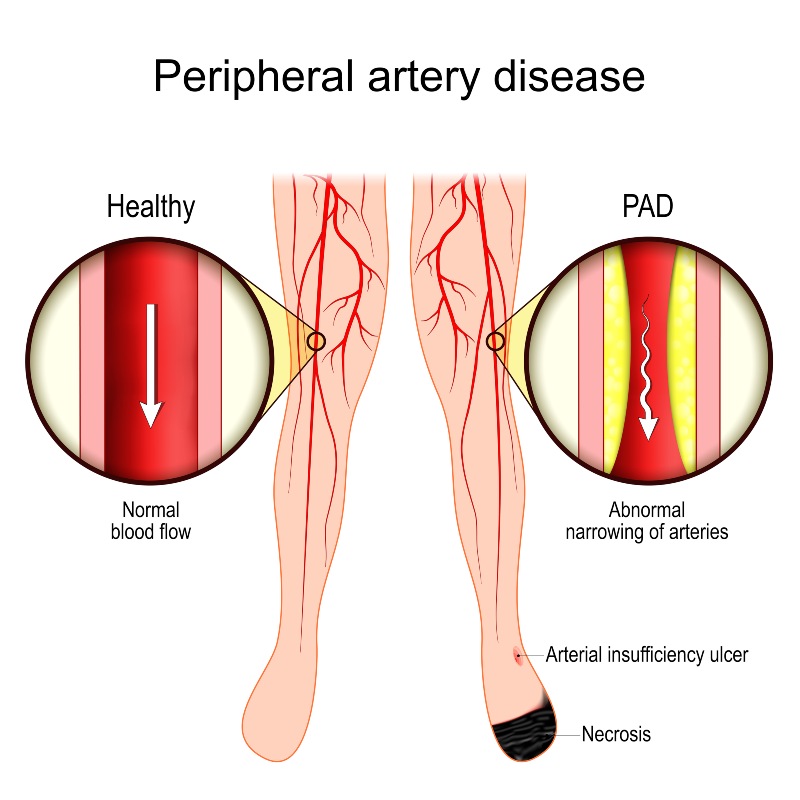
Link Between Diabetes and Peripheral Artery Disease (PAD)
Managing diabetes involves more than just monitoring blood sugar levels. It requires a comprehensive understanding of how the condition impacts your entire vascular system. One of the most critical complications to monitor is Peripheral Artery Disease (PAD). While both conditions are serious on their own, the intersection of diabetes and peripheral artery disease creates a significant health challenge that requires proactive management and early intervention. Arizona Vein & Laser Institute explores the link between diabetes and PAD. Learn more today.
What Is Peripheral Artery Disease?
Peripheral Artery Disease (PAD) is a chronic circulatory condition where narrowed arteries reduce blood flow to the limbs, most commonly the legs. This narrowing is typically caused by atherosclerosis, a process where fatty deposits called plaque build up on the arterial walls over time. As the blood supply diminishes, patients often experience symptoms. If left untreated, the restricted circulation can lead to serious complications, including non-healing sores, tissue death, and a significantly increased risk of systemic cardiovascular events.
How Diabetes Increases PAD Risk
The relationship between PAD and diabetes is deeply rooted in how high blood glucose levels affect the blood vessels. Over time, elevated sugar levels cause damage to the endothelial lining of the arteries. This damage triggers inflammation and accelerates the buildup of plaque, a process known as atherosclerosis. In patients with diabetes, this plaque tends to accumulate more rapidly and extensively in the smaller arteries of the lower legs.
Furthermore, diabetes often coexists with other metabolic issues, such as high blood pressure and abnormal cholesterol levels, both of which further narrow the arteries. This combination severely restricts blood flow to the extremities, leading to chronic diabetic circulation problems that can have devastating consequences if left unaddressed.
Recognizing Peripheral Artery Disease Symptoms
One of the greatest dangers of PAD is that it often remains “silent” until the arterial narrowing is advanced. Paying close attention to PAD warning signs can be life-saving. Common PAD warning signs include:
- Intermittent Claudication – This is the most frequent symptom, characterized by diabetes leg pain or cramping that occurs during physical activity (like walking) and disappears with rest.
- Temperature Changes – One foot or leg may feel significantly colder than the other.
- Skin and Nail Alterations – You may notice shiny skin on the legs, loss of hair on the feet, or brittle toenails that grow slowly.
- Non-healing Sores – Ulcers or wounds on the toes, feet, or legs that heal very slowly or not at all are a major red flag for poor circulation.
- Color Changes – The skin on the legs may turn pale, bluish, or reddish when hanging down.
The Importance of Early Detection and Treatment
Early detection is the cornerstone of preventing the most severe outcomes of PAD, such as critical limb ischemia or amputation. Because diabetic neuropathy can sometimes mask pain, patients with diabetes should undergo regular vascular screenings even if they aren’t experiencing obvious discomfort. Simple, non-invasive tests like the Ankle-Brachial Index (ABI) can effectively measure blood flow and catch the disease in its early stages.
Treatment focuses on managing symptoms to improve mobility and slowing the progression of atherosclerosis to reduce the risk of heart attack and stroke. This often involves a combination of lifestyle modifications and medications to manage blood pressure, cholesterol, and blood sugar. In more advanced cases, minimally invasive procedures like angioplasty or stenting may be necessary to restore blood flow.
Shared Risk Factors Between Diabetes and PAD
The management of PAD is particularly complex in patients with diabetes, as the two conditions share several critical risk factors. The following can accelerate arterial damage:
- Hyperglycemia – Elevated blood glucose levels contribute to endothelial dysfunction and oxidative stress, speeding the progression of atherosclerosis.
- Hypertension – High blood pressure places constant strain on arterial walls, making them more susceptible to plaque accumulation and narrowing.
- Dyslipidemia – Abnormal lipid profiles, common in diabetic patients, lead to higher levels of LDL (“bad”) cholesterol which forms the basis of arterial blockages.
- Chronic Inflammation – Both conditions are characterized by systemic inflammatory states that promote the hardening of the arteries.
- Smoking – Tobacco use significantly compounds the damage caused by diabetes, drastically increasing the likelihood of limb ischemia and poor surgical outcomes.
Lifestyle Changes to Lower PAD and Diabetes Risks
Patients can make lifestyle modifications to help lower PAD and diabetes risks. Some lifestyle changes we recommend include:
- Smoking Cessation – Quitting smoking is the most critical step, as tobacco use severely damages blood vessels and accelerates the progression of both arterial blockages and diabetic complications.
- Glycemic Control – Maintaining blood sugar levels within a target range prevents further nerve and vessel damage, reducing the risk of non-healing ulcers and infections.
- Structured Exercise Programs – Regular physical activity, particularly walking, encourages the development of collateral circulation and improves insulin sensitivity.
- Heart-Healthy Nutrition – Adopting a diet low in saturated fats and sodium helps manage cholesterol levels and blood pressure, slowing the buildup of plaque in the arteries.
- Weight Management – Reducing excess body weight alleviates the physical strain on the lower extremities and helps regulate metabolic function.
Contact Arizona Vein & Laser Institute
Arizona Vein & Laser Institute provides comprehensive vein treatment. If you’re at risk of PAD or have diabetes, it’s vital to prioritize your vascular health. We specialize in regular screening and monitoring to help detect early symptoms of PAD and slow its progression. Take time to proactively manage diabetes and PAD by adopting healthy lifestyle habits. Reach out to us today to schedule a consultation.
